Prenatal Methadone Exposure: Childhood Neurodevelopment Outcomes | Victoria Monnelly | DMCN
[ad_1]source
[ad_2]
Methadone Clinics Near Me – Methadone Clinics NYC – Methadone Clinics USA
Methadone Clinics Near Me – Methadone Clinics NYC – Methadone Clinics USA
[ad_1]
MARSHALLTOWN, Iowa – Andrea Storjohann is glad to see she’s becoming a rarity in rural America.
The nurse practitioner prescribes medication to dozens of patients trying to recover from addiction to heroin or opioid pain relievers.
The general practice where he works, located in a repurposed supermarket building, has no sign designating it as a place where people seek treatment for drug addiction, which is how Storjohann wants it.
“You could come here for OB-GYN care. You could come here for a sore throat. You could come here for any number of reasons,” and no one in the waiting room would know the difference, he said.
Privacy is an important part of treatment. And so is the medication Storjohann prescribes: buprenorphine, which curbs cravings and prevents withdrawal symptoms for people who have stopped abusing opioids. The central Iowa clinic, owned by the nonprofit agency Primary Health Care, has offered buprenorphine since 2016. “We were like a unicorn in this part of the state,” Storjohann said, but that’s changing.
Unlike methadone, the traditional withdrawal drug for heroin or other opioids, buprenorphine can be prescribed in primary care clinics and dispensed at neighborhood pharmacies. Federal and state authorities have encouraged more frontline health care professionals to prescribe Suboxone and other medications containing buprenorphine to patients trying to overcome opioid addiction. Federal regulators have made it easier for doctors, nurse practitioners and physician assistants to become certified to provide the service.
The opioid crisis has deepened over the past decade with the illicit distribution of fentanyl, a powerful and extremely addictive opioid. Its prevalence has complicated the use of drugs to treat opioid addiction. Patients who have misused fentanyl can experience severe withdrawal symptoms when they start taking buprenorphine, so healthcare professionals must be careful when initiating treatment.
In Iowa, officials designated $3.8 million of the state’s initial share of opioid lawsuit settlement money for a University of Iowa program that helps health care providers understand how use the medicines.
Federal agencies are spending millions to expand access to drugs to treat addiction, even in rural areas. The Health Services and Resources Administration, which aims to improve health care for disadvantaged people, offers many of these grants.

Carole Johnson, the agency’s top administrator, said she hopes more training on opioid addiction treatment will encourage health care providers to learn about the latest ways to treat other types of addiction, such as methamphetamine dependence and alcoholism, which many rural states suffer from. “We’re making people aware of substance use disorder in a big way,” he told KHN.
In 2016, only 40 percent of rural counties nationwide had at least one health care provider certified to prescribe buprenorphine, according to a University of Washington study. The study found that this number rose to 63% in 2020.
The study credited the increase to changes in federal regulations that allow nurse practitioners, physician assistants and other mid-level health care providers to prescribe buprenorphine. In the past, only doctors could do this, and many rural counties had no doctors.
Buprenorphine is an opioid that pharmacies most often sell as a tablet or film that dissolves under the tongue. It doesn’t cause the same kind of high as other opioid drugs, but it can prevent the debilitating withdrawal effects experienced with these drugs. Without this help, many people relapse into risky drug use.
The idea of opioid “maintenance treatment” has been around for over 50 years, mostly in the form of methadone. This drug is also an opioid that can reduce the chances of relapsing into heroin or painkiller abuse. But the use of methadone for addiction treatment is strictly regulated, due to concerns that it can be abused.
Only specialist clinics offer methadone maintenance treatment, and most are located in cities. Many patients starting methadone treatment must travel daily to clinics, where staff watch them swallow their medication.
Federal regulators approved Suboxone in 2002, paving the way for addiction treatment in cities without methadone clinics.
Storjohann said buprenorphine offers a practical alternative for Marshalltown, a city of 27,000 surrounded by rural areas.
The practice nurse spends about half of her time working with patients who are taking drugs to prevent relapse into drug abuse. The other half of her practice is mental health care. A recent appointment with patient Bonnie Purk included a bit of both.
Purk, 43, sat in a small exam room with the nurse practitioner, who asked her about her life. Purk described the family struggles and other stressors he faces while trying to abstain from abusing painkillers.
Storjohann asked if Purk felt desperate. “Or are you just frustrated?”
Purk thought for a moment. “I had a week where I was just crying,” she said, wiping her eyes with a tissue. But she said she has not been seriously tempted to relapse.
Storjohann praised her persistence. “You’re riding a roller coaster,” he said. “I think you should give yourself some grace.”
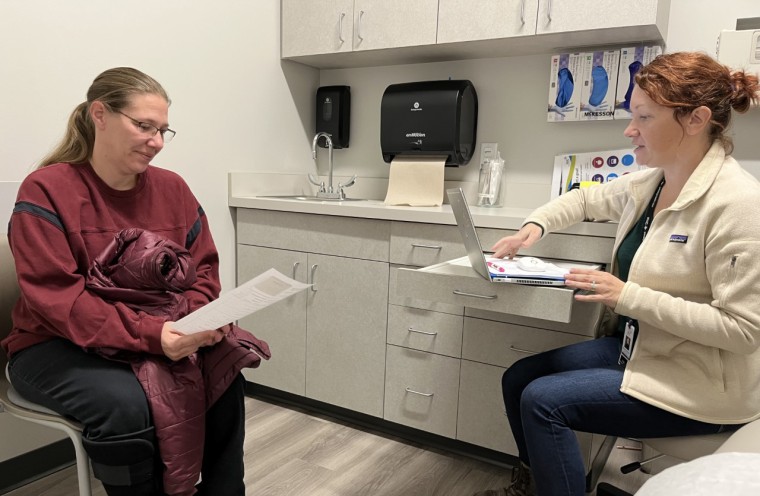 Bonnie Purk, left, meets with nurse Andrea Storjohann at the primary health care clinic in Marshalltown, Iowa.Courtesy Tony Leys/KHN
Bonnie Purk, left, meets with nurse Andrea Storjohann at the primary health care clinic in Marshalltown, Iowa.Courtesy Tony Leys/KHN
Purk knows that Suboxone is not a miracle cure. He has been on the medication for years and has relapsed twice by abusing pain pills. But he has avoided a relapse since the spring and said the medication is helping.
In an interview after his monthly appointment with Storjohann, Purk said the drug dampens cravings and blocks withdrawal symptoms. She recalled terrible night sweats, insomnia, diarrhea and jitters she experienced when trying to stop abusing pills without taking Suboxone.
“Don’t focus on anything but the next solution. ‘Where am I going to get it? How am I going to get it?'” he said. “You just feel like a train wreck, like you’re going to die without him.”
Purk said mental health counseling and frequent drug testing have also helped her stay sober.
Patients may remain on buprenorphine for months or even years. Some skeptics claim that it is trading one drug addiction for another and should not be seen as a substitute for abstinence. But advocates say that skepticism is waning as more families see how treatment can help people regain control of their lives.
Dr. Alison Lynch, a specialist in addiction medicine at the University of Iowa, warned about the risks of fentanyl and buprenorphine at a recent conference for health professionals in training.
Lynch explained that fentanyl stays in the body longer than other opioids, such as heroin. When someone with fentanyl in their system takes buprenorphine, it can cause nausea, muscle pain and other particularly harsh symptoms, he said. “It’s not dangerous. It’s just miserable,” he said, and it can discourage patients from continuing their medication.
Lynch noted that drug dealers are incorporating fentanyl into other drugs, so people don’t always realize they’ve taken it. “I just assume that if people are using any drug that they’ve bought off the street, it’s probably got fentanyl in it,” he said. That’s why, he said, he’s been using smaller starting doses of buprenorphine and increasing the dose more gradually than before.
Nationally, the number of healthcare professionals certified to prescribe buprenorphine has more than doubled in the past four years to more than 134,000, according to the federal Substance Abuse and Mental Health Services Administration. Efforts to expand access to treatment come as drug overdose deaths have more than doubled in the US since 2015, led by overdoses of fentanyl and other opioids.
Storjohann would like to see more general practitioners seek training and certification to prescribe buprenorphine at least occasionally. For example, she said, emergency room doctors might prescribe a few days of the medication for a patient who comes to them in crisis and then refer the patient to a specialist like her. Or a patient’s primary physician might take over buprenorphine treatment after an addiction treatment specialist stabilizes a patient.
Dr. Neeraj Gandotra, chief medical officer of the federal Substance Abuse and Mental Health Services Administration, said he sees potential in expanding these arrangements, known as a “hub and spoke” model of care. Family practice providers who agree to participate would have the assurance that they could always refer a patient to an addiction treatment specialist if problems arose, he said.
Gandotra said he hopes more primary care providers will seek certification to prescribe buprenorphine.
Johnson, the administrator of the Health Resources and Services Administration, said states can also increase access to medication-assisted treatment by expanding their Medicaid programs to provide health insurance coverage to more low-income adults. The federal government pays most of the cost of the Medicaid expansion, but 11 states have declined to do so. That leaves more people without insurance, which means clinics are less likely to be reimbursed for treating them, he said.
Health care providers are no longer required to take special classes to obtain a federal certification — called a “waiver” — to treat up to 30 patients with buprenorphine. But Lynch said even veteran health care professionals could benefit from training on how to properly manage the treatment. “It’s a little daunting to start prescribing a drug that we didn’t get a lot of training on in med school or AP school or nursing school,” he said.
Federal officials have created a public database of health care providers certified to offer buprenorphine treatment for addiction, but the registry only lists providers who agree to include their names. Many don’t. In Iowa, only one-third of certified providers have agreed to be listed in the public registry, according to the Iowa Department of Health and Human Services.
Lynch speculated that some health care professionals want to use the drug to help current patients who need addiction treatment, but aren’t looking to make it a major part of their practice.
Storjohann said some health professionals believe that treating addiction would lead to frustration, because patients can relapse repeatedly. She doesn’t see it that way. “This is a field where people really want to improve,” he said. “It’s really rewarding.”
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism on health issues. Along with policy analysis and surveys, KHN is one of the three main operational programs of KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization that provides information on health issues to the nation.
keep going NBC HEALTH activated Twitter & Facebook.
[ad_2]Methadone Clinics In My Area – Methadone Clinic NYC – Methadone Clinics USA
[ad_1]
 The CITC organizes youth berry picking trips as part of its addiction prevention services. (Photo courtesy of CITC)
The CITC organizes youth berry picking trips as part of its addiction prevention services. (Photo courtesy of CITC)
This summer, the Cook Inlet Tribal Council took youth out berry picking as part of their addiction prevention program.
CITC is a non-profit tribal organization that calls itself a “culturally sensitive social service organization.” Dr. Angela Michaud is CITC’s Senior Director of Recovery Services.
“With our wild blueberries, we didn’t have enough to make [the jam] for the 50 people in the room,” Michaud said. “So we went to Costco and got some blueberries and mixed them with the wild blueberries and made our jam that way.”
She said adapting village traditions to a city like Anchorage helps young people tap into their culture to improve their health outcomes and lower addiction rates.
“Anchorage is a huge town,” Michaud said. “Is [about] get out there and have that sense of connection.”
 A CITC cultural event involves taking young people to pick berries and then giving them a jar to take home to their families. (Photo courtesy of CITC)
A CITC cultural event involves taking young people to pick berries and then giving them a jar to take home to their families. (Photo courtesy of CITC)
Prevention through youth participation
The CITC has found through surveys that participants do not consistently use substances when doing cultural activities.
“That’s a five-hour period where they can say ‘I didn’t drink, I didn’t do alcohol or drugs,’ and they were happy,” Michaud said.
With these promising results, the CITC is using two new federal grants to put Alaska Native cultural education at the forefront of its addiction prevention programs.
“What we do is implement culture for healing [to] prevent tobacco, alcohol, substance use and suicide,” Michaud said.
With a portion of the money, they can organize monthly cultural events aimed at Alaska Native youth and their family members.
Chris Delgado is from an Inupiaq family and serves as a prevention supervisor, directing these activities for the CITC. He grew up in Anchorage.
“I missed some of the cultural activities that were planned,” Delgado said. “It will slowly be forgotten if we don’t stop and do something about it. As long as we can get young people involved, I think we’re in good shape.”
CITC’s prevention activities include more conventional training, such as how to use naloxone, an opioid overdose reversal drug. But it also offers dance lessons, walrus ivory carving, berry picking, traditional storytelling, ice fishing and hooligan net fishing.
 Young people participate in cultural fang carving activities through the CITC program. (Photo courtesy of CITC)
Young people participate in cultural fang carving activities through the CITC program. (Photo courtesy of CITC)
These programs aim to build the confidence of Native youth and teach life skills that participants can learn and share, Michaud said.
A case for connection
A recent article published in a leading medical journal highlighted that teenagers who feel more connected to their community, peers and families are up to 66% less likely to use substances.
Robert Blum of Johns Hopkins University is an expert on adolescent health and the lead author of the paper. He stressed that studies have long shown that conventional information-based youth addiction prevention strategies have no effect on young people and sometimes even have negative effects. He advocates treating “young people as resources, rather than problems.”
CITC has a program that uses youth in long-term recovery as a resource, hiring them to help teach their peers.
“They can share with others what their experiences were to help them succeed in the program,” Michaud said.
Small details, such as offering food options that are part of traditional native diets, bind these communities of peers together.
“People started to get used to eating the salmon, and this year we were finally able to get them out so we could catch it,” he said. “And they got their own fish and brought it in. It’s just the excitement and the stories that came out of it.”
As a result of this program, he cites a decrease in recidivism rates and an increase in participants completing the program and securing jobs and housing.
“We don’t want to just survive,” Michaud said. “We thrive [when] we brought these things to the table. We were overcoming our adversity, and that has a different feel.”
An inverted model
Michaud says many prevention programs take a Western medical curriculum and just add native words to it. But the CITC team has built its entire curriculum on culture. He says that Western models are secondary.
“You’re teaching them to connect with nature and get people outside, away from distractions, drugs, alcohol and abuse,” Michaud said.
And these events are not just occasional meetings. Many youth participants join one event and then continue to sign up for others, even getting involved in other programs CITC offers to increase employment and high school graduation rates.
One group collected seeds and planted them in a community garden. Once they were ripe, the food went to the Alaska Native Health Center so the patients could eat traditional foods.
“And how this relates to our culture is that we’ve had so much trauma in the last two or three generations that it’s taken away a lot of the culture,” Michaud said.
He says Native Americans and Alaskans lived healthy lifestyles for thousands of years and only in the last few hundred years have they had these addiction-related health problems.
“We were good and then we weren’t,” he said. “And now we go back to what we know and we’re good.”
[ad_2]Methadone Clinic Nearby – Methadone Clinics New York City – Methadone Clinics USA
Methadone Clinic Nearby – Methadone Clinic NYC – Methadone Clinics USA
Methadone Clinic Nearby – Methadone Clinic NYC – Methadone Clinics USA
[ad_1]
A monoclonal antibody targeting heroin (11D12) is effective in blocking the euphoric and lethal effects of this widely abused opioid, reported a study in mice by scientists at the Scripps Research Institute in La Jolla, CA. The findings offer a promising new strategy for treating heroin addiction and overdose.
 Kim Janda, PhD, professor of chemistry at Scripps Research is the lead author of the study
Kim Janda, PhD, professor of chemistry at Scripps Research is the lead author of the study
“Our results suggest that a monoclonal antibody-based therapy will be more effective than a vaccine and should target heroin itself rather than its psychoactive metabolites,” said Kim Janda, PhD, Ely R. Callaway, Jr. ., professor of chemistry. , director of Scripps Research’s Worm Institute for Research & Medicine and lead author of the study.
“The work of Dr. Janda and colleagues is very interesting and timely given the importance of developing new strategies to address the opioid epidemic and the dramatic increase in fatal overdoses attributable to opioids or mixtures of opioids and stimulants like cocaine and methamphetamine,” he said. Marco Pravetoni, PhD, a professor in the department of psychiatry and behavioral medicine at the University of Washington School of Medicine, whose team is developing vaccines and monoclonal antibodies (mAbs) against heroin, oxycodone, fentanyl, and analogs of fentanyl. “The results show that target selection is critical to advancing effective therapy.” Pravetoni did not participate in the current study. “
“This work provides compelling data that challenge our current understanding of the pharmacodynamics of heroin. It continues to show the utility of high-affinity antibodies, not only as biological tools, but as viable therapeutics to combat the opioid crisis in course,” said Nicholas Jacob, PhD, senior research scientist at Cessation Therapeutics. Jacob did not participate in the current study.
Political and scientific leaders around the world have been trying to quell the exponentially growing opioid epidemic for decades. However, current medications and behavioral interventions have failed to reduce this public health crisis. Instead, cases of opioid abuse and overdose have increased to unprecedented levels since the start of the COVID-19 pandemic.
Small molecule medications approved by the FDA for opioid use disorders (METADONE, buprenorphine, naltrexone, and naloxone) are limited by adverse side effects, short half-lives, limited availability, high cost, lack of adherence to medication regimen, potential for abuse and relapse to addiction once the medication is discontinued. Immunopharmacotherapy offers a viable alternative. This treatment approach uses antibodies to block the action of illicit substances, keeping the compounds in the peripheral circulation.
Decades of studies have attributed the psychoactive and lethal effects of heroin to its metabolites: 6-monoacetylmorphine (6-AM) and morphine. Therefore, previous immunopharmacotherapeutics have used active and passive vaccines to target heroin metabolites rather than heroin itself. “Passive vaccines” often involve the injection of monoclonal antibodies (mAbs) against the target or its metabolites, while active vaccines use immunostimulatory proteins that mimic the target or its metabolites to activate the patient’s own immune system. However, these therapies have had limited success, underscoring the need to reassess the selection of therapeutic targets.
That the anti-heroin vaccines that Janda’s team and others were developing failed to succeed in clinical trials prompted Janda to step back and assess perceptions and misperceptions in the drug addiction field. drugs
“Most researchers saw heroin as simply a ‘prodrug’ that crosses the blood-brain barrier very quickly and that its ‘prodrug’ ability was simply to transport the major mu opioid receptor drugs, 6-acetylmorphine and , finally, morphine, in the brain.” Janda said. “Based on that reasoning, targeting heroin was an afterthought.”
When previous heroin vaccines failed to counteract the effects of a dose of heroin as expected, poor adjuvants in the vaccine cocktail were pointed to as the culprit.
Janda said, “Actually, the general formulation of the vaccines was correct, but the targeting of 6-acetylmorphine and morphine with the antigen was wrong.”
Building on previous efforts to develop an effective immunopharmacotherapeutic to treat heroin abuse, the current study analyzed four unique mAbs that target heroin, 6-AM, or morphine, or both heroin and 6-AM. The development of these mAbs using a deutero-heroin hapten with broad-spectrum affinity for heroin and its metabolites was reported in a previous study by the same group. The researchers profiled the binding affinities of these mAbs using surface plasmon resonance (SPR), which allowed them to select four different antibody clones with superior abilities to bind heroin or one of the metabolites.
“By using these antibodies, we were able to dissect which of these three drugs was important for (antibody) vaccine development,” Janda said.
The researchers then performed pharmacokinetic assays, overdose assays, and hot-plate and tail-flick assays for pain perception, to identify targets that would effectively neutralize the behavioral, toxic, and lethal effects of heroin. These in vitro and in vivo tests showed that mAb 11D12 targeting heroin was, unexpectedly, the optimal therapeutic to suppress the effects of heroin, compared to the other mAbs that targeted its two main metabolites.
 This study reveals that the monoclonal antibody 11D12 abolishes the psychoactive and lethal effects of heroin in mice. [Adapted from Lee et al., ACS Central Science]The authors showed that 11D12 blocks the analgesic effects of heroin and prevents heroin from slowing breathing and heart rate, the direct causes underlying heroin’s lethality. mAb 11D12 achieved this with a high degree of potency required for human clinical trials.
This study reveals that the monoclonal antibody 11D12 abolishes the psychoactive and lethal effects of heroin in mice. [Adapted from Lee et al., ACS Central Science]The authors showed that 11D12 blocks the analgesic effects of heroin and prevents heroin from slowing breathing and heart rate, the direct causes underlying heroin’s lethality. mAb 11D12 achieved this with a high degree of potency required for human clinical trials.
Pravetoni said, “Lee et al., provide evidence that mAb can be used to reverse opioid overdose and to reduce lethality after exposure. These results are consistent with our work on anti-opioid mAbs (Baehr et al., JPET 2020; Baehr et al., JPET 2022; Hicks et al., HVI 2022) and support the idea that the vaccine and mAb warrant clinical investigation.”
In addition, the researchers found that 11D12 remained active in circulation for weeks, unlike previous therapies that were cleared from circulation within hours. This is a key advantage against poor patient adherence to treatment regimens, which is common among patients with addiction.
The effectiveness of 11D12 in counteracting the effects of heroin surprised Janda and his team because, unlike the other three antibodies tested, it targets heroin with the highest binding affinity and does not to its metabolites. Because esterase enzymes in the blood rapidly convert heroin to morphine and 6-acetylmorphine through sequential deacetylation, scientists have so far identified the metabolites as better targets.
“The focus on metabolites fundamentally misled the field: our report will reset research in a direction where successful clinical trials can now be achieved,” said Janda. The current findings shed light on the reasons underlying the failure of previous attempts to develop therapeutics targeting only heroin metabolites.
“From work in the field, we know that targeting heroin, 6 AM, and morphine may be equally important. However, the impact of individual vaccines or mAb formulations remains to be assessed eventually in human subjects through clinical trials,” said Pravetoni. “For example, targeting heroin and 6-AM would be important to reduce the acute toxicity and reward of heroin, but it is unclear whether targeting morphine would also be necessary to counteract the chronic effects of heroin metabolites. heroin in patients with OUD”.
“We are always trying to optimize the ability of opioids and other drugs of abuse to generate antibodies, as high levels of antibodies are needed to counteract the toxic and lethal effects of drugs of abuse, especially fentanyl-related opioids.” , said Thomas Kosten. , MD, the Wagoner Professor of Psychiatry, Pharmacology, Neuroscience and Immunology at Baylor College of Medicine. “While this work focuses on heroin and this class of opioids, similar work by this research group has greatly contributed to our ability to develop vaccines and monoclonals for other classes of drugs of abuse, including fentanyl-related opioids, which are the most lethal and resistant. to our existing FDA-approved treatments of methadone, buprenorphine, and depot naltrexone. This article provides an excellent contribution to our field of immunotherapy for addictions”. Kosten did not participate in the current study.
In future studies, the team will test a human version of the mouse monoclonal antibody 11D12 and parallel mAbs to neutralize the synthetic opioids fentanyl, carfentanil, and other related compounds.
Janda said, “Our heroin antibody could, in theory, have translational value for clinical trials if humanized.”
[ad_2]Methadone Clinics Nearby – Methadone Clinics NYC – Methadone Clinics USA