[ad_1]
MARSHALLTOWN, Iowa – Andrea Storjohann is glad to see she’s becoming a rarity in rural America.
The nurse practitioner prescribes medication to dozens of patients trying to recover from addiction to heroin or opioid pain relievers.
The general practice where he works, located in a repurposed supermarket building, has no sign designating it as a place where people seek treatment for drug addiction, which is how Storjohann wants it.
“You could come here for OB-GYN care. You could come here for a sore throat. You could come here for any number of reasons,” and no one in the waiting room would know the difference, he said.
Privacy is an important part of treatment. And so is the medication Storjohann prescribes: buprenorphine, which curbs cravings and prevents withdrawal symptoms for people who have stopped abusing opioids. The central Iowa clinic, owned by the nonprofit agency Primary Health Care, has offered buprenorphine since 2016. “We were like a unicorn in this part of the state,” Storjohann said, but that’s changing.
Unlike methadone, the traditional withdrawal drug for heroin or other opioids, buprenorphine can be prescribed in primary care clinics and dispensed at neighborhood pharmacies. Federal and state authorities have encouraged more frontline health care professionals to prescribe Suboxone and other medications containing buprenorphine to patients trying to overcome opioid addiction. Federal regulators have made it easier for doctors, nurse practitioners and physician assistants to become certified to provide the service.
The opioid crisis has deepened over the past decade with the illicit distribution of fentanyl, a powerful and extremely addictive opioid. Its prevalence has complicated the use of drugs to treat opioid addiction. Patients who have misused fentanyl can experience severe withdrawal symptoms when they start taking buprenorphine, so healthcare professionals must be careful when initiating treatment.
In Iowa, officials designated $3.8 million of the state’s initial share of opioid lawsuit settlement money for a University of Iowa program that helps health care providers understand how use the medicines.
Federal agencies are spending millions to expand access to drugs to treat addiction, even in rural areas. The Health Services and Resources Administration, which aims to improve health care for disadvantaged people, offers many of these grants.

Carole Johnson, the agency’s top administrator, said she hopes more training on opioid addiction treatment will encourage health care providers to learn about the latest ways to treat other types of addiction, such as methamphetamine dependence and alcoholism, which many rural states suffer from. “We’re making people aware of substance use disorder in a big way,” he told KHN.
In 2016, only 40 percent of rural counties nationwide had at least one health care provider certified to prescribe buprenorphine, according to a University of Washington study. The study found that this number rose to 63% in 2020.
The study credited the increase to changes in federal regulations that allow nurse practitioners, physician assistants and other mid-level health care providers to prescribe buprenorphine. In the past, only doctors could do this, and many rural counties had no doctors.
Buprenorphine is an opioid that pharmacies most often sell as a tablet or film that dissolves under the tongue. It doesn’t cause the same kind of high as other opioid drugs, but it can prevent the debilitating withdrawal effects experienced with these drugs. Without this help, many people relapse into risky drug use.
The idea of opioid “maintenance treatment” has been around for over 50 years, mostly in the form of methadone. This drug is also an opioid that can reduce the chances of relapsing into heroin or painkiller abuse. But the use of methadone for addiction treatment is strictly regulated, due to concerns that it can be abused.
Only specialist clinics offer methadone maintenance treatment, and most are located in cities. Many patients starting methadone treatment must travel daily to clinics, where staff watch them swallow their medication.
Federal regulators approved Suboxone in 2002, paving the way for addiction treatment in cities without methadone clinics.
Storjohann said buprenorphine offers a practical alternative for Marshalltown, a city of 27,000 surrounded by rural areas.
The practice nurse spends about half of her time working with patients who are taking drugs to prevent relapse into drug abuse. The other half of her practice is mental health care. A recent appointment with patient Bonnie Purk included a bit of both.
Purk, 43, sat in a small exam room with the nurse practitioner, who asked her about her life. Purk described the family struggles and other stressors he faces while trying to abstain from abusing painkillers.
Storjohann asked if Purk felt desperate. “Or are you just frustrated?”
Purk thought for a moment. “I had a week where I was just crying,” she said, wiping her eyes with a tissue. But she said she has not been seriously tempted to relapse.
Storjohann praised her persistence. “You’re riding a roller coaster,” he said. “I think you should give yourself some grace.”
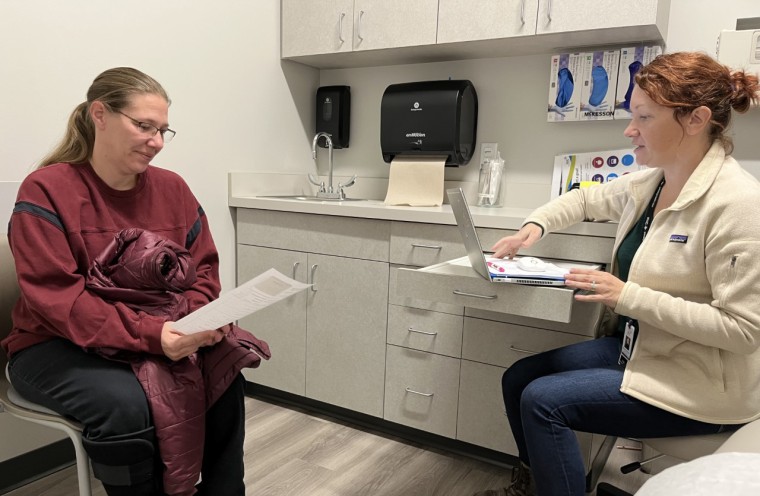 Bonnie Purk, left, meets with nurse Andrea Storjohann at the primary health care clinic in Marshalltown, Iowa.Courtesy Tony Leys/KHN
Bonnie Purk, left, meets with nurse Andrea Storjohann at the primary health care clinic in Marshalltown, Iowa.Courtesy Tony Leys/KHN
Purk knows that Suboxone is not a miracle cure. He has been on the medication for years and has relapsed twice by abusing pain pills. But he has avoided a relapse since the spring and said the medication is helping.
In an interview after his monthly appointment with Storjohann, Purk said the drug dampens cravings and blocks withdrawal symptoms. She recalled terrible night sweats, insomnia, diarrhea and jitters she experienced when trying to stop abusing pills without taking Suboxone.
“Don’t focus on anything but the next solution. ‘Where am I going to get it? How am I going to get it?'” he said. “You just feel like a train wreck, like you’re going to die without him.”
Purk said mental health counseling and frequent drug testing have also helped her stay sober.
Patients may remain on buprenorphine for months or even years. Some skeptics claim that it is trading one drug addiction for another and should not be seen as a substitute for abstinence. But advocates say that skepticism is waning as more families see how treatment can help people regain control of their lives.
Dr. Alison Lynch, a specialist in addiction medicine at the University of Iowa, warned about the risks of fentanyl and buprenorphine at a recent conference for health professionals in training.
Lynch explained that fentanyl stays in the body longer than other opioids, such as heroin. When someone with fentanyl in their system takes buprenorphine, it can cause nausea, muscle pain and other particularly harsh symptoms, he said. “It’s not dangerous. It’s just miserable,” he said, and it can discourage patients from continuing their medication.
Lynch noted that drug dealers are incorporating fentanyl into other drugs, so people don’t always realize they’ve taken it. “I just assume that if people are using any drug that they’ve bought off the street, it’s probably got fentanyl in it,” he said. That’s why, he said, he’s been using smaller starting doses of buprenorphine and increasing the dose more gradually than before.
Nationally, the number of healthcare professionals certified to prescribe buprenorphine has more than doubled in the past four years to more than 134,000, according to the federal Substance Abuse and Mental Health Services Administration. Efforts to expand access to treatment come as drug overdose deaths have more than doubled in the US since 2015, led by overdoses of fentanyl and other opioids.
Storjohann would like to see more general practitioners seek training and certification to prescribe buprenorphine at least occasionally. For example, she said, emergency room doctors might prescribe a few days of the medication for a patient who comes to them in crisis and then refer the patient to a specialist like her. Or a patient’s primary physician might take over buprenorphine treatment after an addiction treatment specialist stabilizes a patient.
Dr. Neeraj Gandotra, chief medical officer of the federal Substance Abuse and Mental Health Services Administration, said he sees potential in expanding these arrangements, known as a “hub and spoke” model of care. Family practice providers who agree to participate would have the assurance that they could always refer a patient to an addiction treatment specialist if problems arose, he said.
Gandotra said he hopes more primary care providers will seek certification to prescribe buprenorphine.
Johnson, the administrator of the Health Resources and Services Administration, said states can also increase access to medication-assisted treatment by expanding their Medicaid programs to provide health insurance coverage to more low-income adults. The federal government pays most of the cost of the Medicaid expansion, but 11 states have declined to do so. That leaves more people without insurance, which means clinics are less likely to be reimbursed for treating them, he said.
Health care providers are no longer required to take special classes to obtain a federal certification — called a “waiver” — to treat up to 30 patients with buprenorphine. But Lynch said even veteran health care professionals could benefit from training on how to properly manage the treatment. “It’s a little daunting to start prescribing a drug that we didn’t get a lot of training on in med school or AP school or nursing school,” he said.
Federal officials have created a public database of health care providers certified to offer buprenorphine treatment for addiction, but the registry only lists providers who agree to include their names. Many don’t. In Iowa, only one-third of certified providers have agreed to be listed in the public registry, according to the Iowa Department of Health and Human Services.
Lynch speculated that some health care professionals want to use the drug to help current patients who need addiction treatment, but aren’t looking to make it a major part of their practice.
Storjohann said some health professionals believe that treating addiction would lead to frustration, because patients can relapse repeatedly. She doesn’t see it that way. “This is a field where people really want to improve,” he said. “It’s really rewarding.”
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism on health issues. Along with policy analysis and surveys, KHN is one of the three main operational programs of KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization that provides information on health issues to the nation.
keep going NBC HEALTH activated Twitter & Facebook.
[ad_2]Source: As Overdoses Rise in Rural America, More Doctors Prescribe Addiction Drugs
Methadone Clinics In My Area – Methadone Clinic NYC – Methadone Clinics USA















